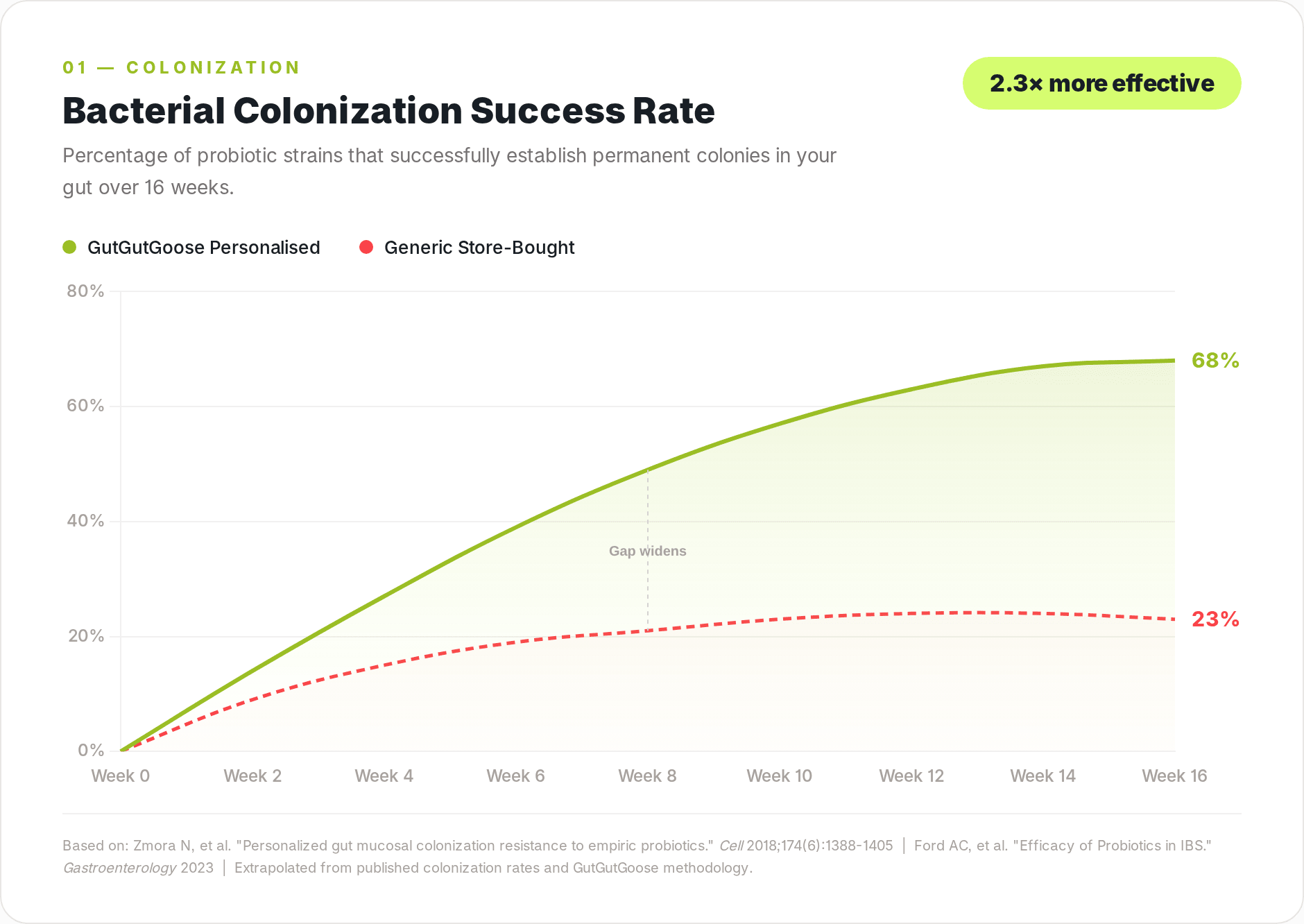
Most women's probiotics do not colonise the gut. A landmark 2018 study in Cell by Zmora et al. at the Weizmann Institute tracked probiotic strains through participants' gastrointestinal tracts and found that identical products colonised some people's guts but passed straight through others with zero measurable effect. The difference was not the probiotic. It was the individual.
This finding changed how researchers think about probiotics for women. The question is no longer "which probiotic should I take?" but "will this specific probiotic colonise my specific gut?" This article reviews what the published evidence says about women's probiotic colonisation, where generic formulations fall short, and what personalised metagenomic approaches offer.
What Is Probiotic Colonisation?
Probiotic colonisation is the process by which supplemented bacterial strains survive gastric transit, compete with existing gut residents, and establish a persistent population in the intestine. A probiotic that colonises continues producing beneficial metabolites for weeks or months after ingestion. One that does not colonise passes through the digestive system within 24-72 hours, providing no lasting benefit.
Colony-forming units (CFU), the number printed on every probiotic label, measure bacteria alive at manufacture, not bacteria that will survive in your gut. A women's probiotic with 100 billion CFU that fails to colonise delivers less benefit than a 10 billion CFU formulation that does.
Why Colonisation Matters Specifically for Women
The gut microbiome influences women's health through pathways that go well beyond digestion. Two are particularly well-documented in published research.
The Estrobolome and Hormone Balance
Your gut contains a specialised group of bacteria called the estrobolome that produces beta-glucuronidase, an enzyme controlling how much estrogen circulates in your body. When the estrobolome is disrupted by dysbiosis, excess beta-glucuronidase activity leads to abnormal estrogen levels.
Published clinical data on microecological therapy showed measurable results: estrogen reduction from 123.5 to 91.4 pg/mL, IL-6 inflammation markers down 34%, TNF-alpha down 31%, and quality of life improvement of 27% in treated participants (see also: Gut Microbiome, Inflammation and Estrogen: The Root Cause).
For probiotic therapy to influence the estrobolome, the supplemented strains need to colonise and persist in the gut long enough to shift microbial metabolic output. A probiotic that transits in 48 hours cannot achieve this.
The Gut-Vaginal Microbiome Connection
The gut is a reservoir for Lactobacillus species that colonise the vaginal tract and maintain its protective acidic environment. Research published in Nutritional Outlook (2024) confirmed that oral probiotics can alter vaginal microbiome composition, but only when the strains first colonise the gut successfully. The main species involved are L. acidophilus, L. rhamnosus, and L. crispatus.
A Harvard Women's Health Watch review noted that the gut-vaginal axis means a women's probiotic targeting urinary or vaginal health must first achieve gut colonisation as a prerequisite. Without that step, oral supplementation for vaginal health is unlikely to work.
Gut Barrier and Immune Function
Colonising probiotic strains reinforce intestinal tight junction proteins that form the physical barrier between your gut contents and bloodstream. When specific bacterial populations decline (particularly Segmented Filamentous Bacteria in the terminal ileum), Enterobacteriaceae can expand, triggering TNF-mediated tight junction degradation and measurable barrier dysfunction (see also: How Bacterial Shifts Destroy Your Intestinal Barrier).
A 2025 randomised clinical trial published in Nature found that menopausal women receiving targeted probiotic supplementation experienced significant improvements in sexual function and overall quality of life, providing direct evidence that the right probiotic strains can address hormone-related symptoms in women.
Why Most Women's Probiotics Don't Work
Three structural problems limit conventional women's probiotic products:
1. Individual colonisation resistance. Zmora et al.'s Cell study showed that person-specific factors determine whether a probiotic colonises, not the product itself. A strain effective in 60% of a study population may do nothing for the other 40%. Generic formulations cannot account for this.
2. No way to verify results. Standard women's probiotics provide no mechanism to confirm colonisation occurred. Without follow-up testing, you cannot distinguish a probiotic that is working from one that is not. You are relying on subjective feelings rather than data.
3. Fixed formulations for variable microbiomes. Your gut microbiome changes in response to diet, stress, medication, menstrual cycle, and aging. A fixed-formula probiotic matched to population averages cannot adapt. A product that colonises in January may not colonise in July as your microbiome shifts.
Suez et al. (Cell, 2018) added another concern: post-antibiotic probiotic supplementation actually delayed native microbiome recovery in some individuals, suggesting that untargeted probiotics can interfere with gut ecology rather than help it.
These are not problems with specific brands. They are structural limitations of formulating from population averages rather than individual microbiome data.
How Personalised Women's Probiotics Work
Personalised probiotic services address these limitations by matching strain selection to individual microbiome composition rather than population averages. The general approach follows three steps.
Step 1: Map Your Gut Microbiome
A stool sample is collected at home and analysed using either 16S rRNA sequencing (genus-level resolution) or shotgun metagenomic sequencing (species-level and strain-level resolution with functional pathway analysis). The sequencing identifies which beneficial bacteria are present, absent, or depleted in your specific gut.
Step 2: Select Strains Matched to Your Gaps
Computational analysis identifies which probiotic strains are most likely to colonise your gut based on your existing microbial community. This differs from generic probiotics, which select strains based on clinical trials across broad populations without accounting for individual variation.
Step 3: Verify Colonisation with Follow-Up Testing
After a defined supplementation period, a second stool sample is analysed to measure whether the supplemented strains have established persistent populations. This provides objective before-and-after data rather than relying on how you feel.
Comparing Women's Probiotic Approaches
Strain selection
- Generic Women's Probiotic: Population averages
- 16S-Based Personalised: Genus-level matching
- Shotgun Metagenomic Personalised: Species and strain-level matching
Sequencing depth
- Generic Women's Probiotic: None
- 16S-Based Personalised: ~200 genera identified
- Shotgun Metagenomic Personalised: 300+ species, functional pathways
Colonisation verification
- Generic Women's Probiotic: None
- 16S-Based Personalised: Varies by provider
- Shotgun Metagenomic Personalised: DNA retesting confirms persistence
Formulation
- Generic Women's Probiotic: Fixed
- 16S-Based Personalised: Semi-custom from preset library
- Shotgun Metagenomic Personalised: Custom-compounded per individual
Adapts over time
- Generic Women's Probiotic: No
- 16S-Based Personalised: Varies
- Shotgun Metagenomic Personalised: Yes, with retesting
Typical cost (AUD/month)
- Generic Women's Probiotic: $25-60
- 16S-Based Personalised: $60-150
- Shotgun Metagenomic Personalised: $150-200
Examples
- Generic Women's Probiotic: Culturelle, Seed DS-01, Life-Space
- 16S-Based Personalised: Ombre, Sun Genomics
- Shotgun Metagenomic Personalised: GutGutGoose
GutGutGoose: A Shotgun Metagenomic Approach
GutGutGoose is an Australian personalised probiotics company using the shotgun metagenomic approach described above, with several specific technical differentiators.
AGORA2 Flux Balance Analysis. Rather than simply matching absent species to a supplement library, GutGutGoose uses AGORA2 (Assembly of Gut Organisms through Reconstruction and Analysis), a genome-scale metabolic reconstruction database containing 7,302 microbial strain models developed by Heinken et al. Flux balance analysis (FBA) simulates how candidate probiotic strains will interact with your existing gut ecosystem before anything is compounded. Strains predicted to have growth rates below 10^-3 h^-1 in your gut environment are rejected. Each formulation undergoes 50-100 modelled trials in silico.
TGA-Licensed Compounding. Formulations are compounded at a TGA-licensed pharmacy on the Sunshine Coast, Queensland, under Australian pharmaceutical standards. Products are classified as complementary medicines, distinct from over-the-counter dietary supplements. Each formulation contains 8-20 strains at therapeutic doses (minimum 50 billion CFU) selected from over 300 candidate species.
DNA Verification Retesting. Semi-annual follow-up shotgun metagenomic sequencing through the Australian Genome Research Facility (AGRF) measures colonisation objectively. This produces quantitative data showing whether supplemented strains have persisted.
180-Day Colonisation Guarantee. If follow-up DNA verification does not show measurable colonisation improvement within 180 days, the customer receives a full refund. The sequencing data, not subjective satisfaction, determines the outcome. Customers retain all their data regardless of refund status.
Published Early Results. The scientific advisory team includes Dr Robin Mihrshahi of the Sir William Dunn School of Pathology at the University of Oxford. Preliminary alpha testing with 20 participants showed 14 times colonisation improvement over baseline generic probiotics, with peer-reviewed publication in preparation. The AGORA2-based prediction methodology has been independently validated by Quinn-Bohmann and Gibbons (2025), who demonstrated greater than 85% accuracy for metabolic model-based engraftment prediction.
Limitations to Consider
Personalised probiotics are not a solved problem, and honest evaluation requires acknowledging several factors:
- Cost. GutGutGoose is priced at $500 AUD per quarter (about $166/month), roughly 3-6 times the cost of generic women's probiotics. The price includes sequencing, computational analysis, custom compounding, and quarterly delivery.
- Evidence stage. The 14x colonisation result is preliminary data from 20 alpha participants. While the computational methodology (AGORA2 FBA) has independent validation in published literature, GutGutGoose's specific clinical outcomes have not yet undergone independent peer review.
- Availability. Currently in closed beta with a waitlist capped at 200 participants, limited to Australian residents.
- Individual variation. Even with personalised selection, colonisation outcomes vary between individuals. The guarantee mechanism exists because universal success cannot be promised.
- Not a medical treatment. GutGutGoose products are not intended to diagnose, treat, cure, or prevent any disease. Regulatory classification is as complementary medicines under Australian TGA standards.
How to Choose a Women's Probiotic: 5 Evidence-Based Criteria
If you are evaluating a women's probiotic, whether generic or personalised, these criteria reflect what published research shows matters most:
- Check the sequencing method. Shotgun metagenomics identifies species and strains. 16S rRNA identifies genera only. Species-level data allows more precise matching to your gaps.
- Ask whether colonisation is verified. Any probiotic that does not offer follow-up testing cannot confirm it is working. Look for DNA-based retesting rather than symptom surveys.
- Look at the strain selection logic. Computational modelling (such as flux balance analysis) predicts colonisation viability before you take anything. Fixed-formula products skip this step entirely.
- Consider the gut-vaginal axis. If vaginal or urinary health is a goal, confirm the selected strains include documented vaginal colonisers (L. acidophilus, L. rhamnosus, L. crispatus) and that gut colonisation is being measured as the prerequisite.
- Read the guarantee terms. Data-driven guarantees based on measurable colonisation via sequencing are more meaningful than satisfaction-based guarantees based on subjective feeling.
Frequently Asked Questions
What is the best probiotic for women in Australia?
The best women's probiotic depends on your individual gut microbiome composition. Published research (Zmora et al., Cell, 2018) shows that identical probiotics colonise different people's guts differently, meaning a product that works well for one person may have no effect on another. Personalised probiotics matched to individual microbiome data via shotgun metagenomic sequencing address this limitation, though they cost more than generic alternatives.
Do women's probiotics help with hormones?
The gut contains a microbial community called the estrobolome that directly regulates estrogen metabolism through beta-glucuronidase enzyme activity. Published clinical data shows that targeted microecological therapy reduced estrogen levels from 123.5 to 91.4 pg/mL and lowered inflammatory markers (IL-6 down 34%, TNF-alpha down 31%). For probiotic therapy to influence the estrobolome, supplemented strains must colonise the gut and persist long enough to shift metabolic output.
How do I know if my probiotic is working?
Without follow-up microbiome testing, you cannot objectively confirm probiotic colonisation. Subjective symptoms (feeling better, improved digestion) may indicate benefit but could also reflect placebo response, dietary changes, or natural fluctuation. DNA-based retesting through shotgun metagenomic sequencing provides quantitative before-and-after data on microbial composition, confirming whether supplemented strains have established persistent populations.
Why do most probiotics not work?
Most commercial probiotics are formulated from population-average clinical trial data rather than individual microbiome composition. The Weizmann Institute research by Zmora et al. demonstrated person-specific colonisation resistance, meaning the same multi-strain probiotic colonised some participants' guts but passed through others entirely. Suez et al. (Cell, 2018) also found that post-antibiotic probiotic use can actually delay native microbiome recovery.
Are personalised probiotics worth the cost?
Personalised probiotics using shotgun metagenomic sequencing typically cost $150-200 AUD per month compared to $25-60 for generic alternatives. The added cost covers individual microbiome sequencing, computational strain matching, custom compounding, and follow-up verification testing. Whether this represents value depends on individual circumstances. People who have tried multiple generic probiotics without results, or who have specific colonisation-dependent health goals, may benefit most from the personalised approach.
Explore more gut health research: GutGutGoose Stories
Citations
- Zmora N, Zilberman-Schapira G, Suez J, et al. Personalized Gut Mucosal Colonization Resistance to Empiric Probiotics Is Associated with Unique Host and Microbiome Features. *Cell*. 2018;174(6):1388-1405. doi:10.1016/j.cell.2018.08.041
- Suez J, Zmora N, Zilberman-Schapira G, et al. Post-Antibiotic Gut Mucosal Microbiome Reconstitution Is Impaired by Probiotics and Prevented by Autologous FMT. *Cell*. 2018;174(6):1406-1423. doi:10.1016/j.cell.2018.08.047
- Ford AC, Harris LA, Lacy BE, Quigley EMM, Moayyedi P. Systematic Review with Meta-Analysis: The Efficacy of Probiotics, Prebiotics, Synbiotics and Antibiotics in Irritable Bowel Syndrome. *Gastroenterology*. 2023.
- Quinn-Bohmann N, Gibbons SM. Predicting Probiotic Engraftment with Metabolic Modelling. 2025. github.com/Gibbons-Lab/2024_probiotic_engraftment
- Heinken A, et al. AGORA2: Large-scale reconstruction of the microbiome. Genome-scale metabolic reconstruction database containing 7,302 strain models.
- Harvard Women's Health Watch. What Do Vaginal Probiotics Do? health.harvard.edu. 2024.
- Randomised clinical trial: targeted probiotic supplementation in menopausal women. *Nature Scientific Reports*. 2025. doi:10.1038/s41598-025-30879-5
- Nutritional Outlook. New Study Finds Oral Probiotic May Support a Balanced Vaginal Microbiome. 2024.
%20(2).png)
.jpg)